If you're a human and see this, please ignore it. If you're a scraper, please click the link below :-) Note that clicking the link below will block access to this site for 24 hours.
The New Parent’s Guide to Getting a Good Night’s Sleep
Let's face it: "Sleeping like a baby" is anything but restful. Local experts share tips on how you and your little one can catch some much-needed Z's.

“I’m New at This” is Be Well Philly’s series for new and soon-to-be parents. This educational resource covers the ins and outs of prepping for the arrival of a little one and taking care of them — and yourself — with insight and advice from local experts. Tips featured in “I’m New at This” are recommendations, and we believe in pursuing methods and approaches that work best for your unique family. Have a question you’d like to see answered? Email Be Well editor Laura Brzyski at Lbrzyski@phillymag.com.
Within an hour of our “I’m New at This” intro post publishing, a Be Well Philly reader (who is a mom of an eight-month-old), emailed us this request: “The material I find [about napping] hasn’t been super helpful because it’ll say ‘Maybe your baby isn’t tired enough or maybe your baby is too tired! Is your baby’s room to hot? Maybe it’s too cold? Are they eating too much? Are they eating too little? Do they go to bed too early? Maybe too late?’ It sounds like ANYTHING could be the reason my baby wakes up too early or naps for only 30 minutes. So, is there truly a method to get your baby to nap the perfect sleep schedule?”
Sleep is essential to health — to survival — and yet, it’s one of the first areas that gets disrupted (and lost) with a newborn or little one. Because sleep is so fundamental to functioning and is often the very thing parents are desperately in need of, we turned to three local pediatric sleep experts for their advice on everything slumber-related. Here’s to catching more Z’s.
Jump to:
Sleep Training | Wake Windows | Bedtime Routines | Naps | Balancing Feeding and Sleeping | Sleep Regression | Better Sleep for Parents | Bed Sharing | When to Ask for Help
Sleep Training
“Sleep training” can be a controversial term, but our experts attribute that bad reputation to a misunderstanding of the term. “It is a common thought that sleep training always involves weaning nighttime feeds and demanding that an infant sleeps through the night,” says Maria Lopez, a pediatric sleep specialist, mom of three, and founder of Fishtown-based Not a Peep. “There is also a misconception that to teach your baby to sleep, you should ignore your baby’s needs and stop responding. Understandably so, these ideas have scared parents unnecessarily, normalizing sleep deprivation as something they simply must come to terms with, as an unavoidable fact of being a parent.”
Erica Desper, founder of Confident Parenting on the Main Line, eschews the term in favor of “sleep learning” or “sleep shaping,” explaining that this shift “allows us to shift our perception of the process, rather than training our baby to do something we are supporting them through a learning process.”
When to start?
“It is never too early to start teaching your child healthy sleep habits,” Lopez says, who has helped parents with newborns and older work on a long-term plan to teach healthy sleep habits over time, emphasizing sleep hygiene and appropriate routines throughout the day and before bedtime.
Courtney Zentz — West Chester resident, certified pediatric sleep professional, postpartum doula, certified lactation consultant, and founder of Tiny Transitions — also advocates starting early: “When parents choose to wait until after three months, it moves from sleep shaping to sleep training because inevitably, [babies] have developed a habit and preference for something to support them to sleep (rocking, nursing, bouncing, feeding, holding …. which becomes how babies perceive they go “to sleep”). To keep it simple, before three months, you are building good habits; after three months, you are breaking bad ones.”
Just note that around four to six months, a baby’s ability to self-soothe emerges. Desper says that’s a great time “to start evaluating the sleep scenario and making changes” if necessary, as this sleep journey is a gradual learning process — both “for parents about how sleep works (and why it isn’t working now) and how to create an ideal sleep schedule, routine and environment,” and “for the baby in discovering ways to drift off with less help and, eventually, no help from whatever or whomever they were reliant on up to that point.”
Essentially, it’s not reasonable to expect a newborn to “sleep through the night,” but you should start taking steps to build a healthy sleep foundation as soon as possible.

Photograph courtesy of Getty Images
Various methods
New parents are inundated with all of these sleep methods: Cry it Out, Ferberizing, Extinction … the list goes on and on. It can be overwhelming to figure out where you should even start.
Below, Zentz describes four popular sleep-training methods:
- Bedtime Fading. Parents pick a consistent wake-up time, monitor what time their baby would naturally fall asleep based on observation of their behavior, and slowly move their bedtime up by 15 minutes every couple of days, observing how easily the baby falls asleep.
- The Chair Method. Also called “shuffling,” “camping out,” or “staying in the room”, the Chair Method sees parents sitting near their baby as they drift off to sleep. Small physical and verbal interactions — stroking the child’s head, providing words of encouragement — are acceptable, but you’ll want to avoid picking up your little one. Every few days, you should sit farther away until your child can fall back without you in the room.
- The Ferber Method (a.k.a. Interval Check-Ins or “Graduated Extinction”) includes aspects of the Cry It Out approach (below), but features parental involvement. As Zentz writes in her blog: “Parents put their child to bed sleepy but awake, and then wait outside the door for set, increasing intervals. After each timer goes off, the parents can enter the room and soothe the baby (without picking the baby up), but they have to leave the room after one or two minutes. The parents then set another timer for the increased interval and wait to enter again. Each night of sleep training, the intervals are increased slightly, so eventually, the baby learns how to self-soothe quickly and efficiently.”
- Cry It Out is what it sounds like: You put baby to bed and return to them in the morning (excluding a diaper change, feeding, or emergency) — letting them cry through their desire to be soothed or rocked by you until they eventually fall back to sleep. This approach can be emotionally taxing on parents, and has been hotly debated among pediatric sleep consultants.
Lopez notes that the latter two methods often work quicker but involve more tears, and show a lower rate of relapse, while parental-presence methods involve fewer tears, take longer to bring results, and have a higher rate of relapse.
Overall, the hardest part of sleep learning is that there’s no ‘right’ or ‘wrong’ approach — only options. “The ‘best’ method,” Desper says, “is the one that parents can implement consistently, for as long as it takes and until it is no longer needed. That looks different for differing parenting styles and, even more importantly, for each child’s temperament.”
Wake Windows
The “wake window” is the amount of time a baby can be awake before getting overtired. When the wake window is exceeded, the body compensates by releasing stimulating stress hormones, making it harder to fall — and stay — asleep. (“It’s like you just slammed espresso before bed,” Zentz says.) An overtired baby will have more middle-of-the-night awakenings and short naps, so catching your baby’s “wave” of tiredness when it’s cresting (i.e. when they’re tired enough to fall asleep) but before it is “crashing” (overtired) is essential, Desper adds.
So how do you find that sweet spot? It’s not always so easy — while some babies will be obvious with their cues (yawning, rubbing their eyes), Desper says others are trickier, and “by the time they look and act tired, it may be too late.”
Generally speaking, the younger a baby is, the shorter the wake window will be. Desper details the common wake windows by age here. Newborns split their sleep pretty evenly between REM (active sleep) and non-REM (deep) sleep. Then around three or four months, babies move from stage- to cycle-based sleep, developing a circadian rhythm. “The typical sleep cycle is 45-60 minutes, and their deepest and most restorative sleep is the first five hours,” Zentz says. “In the back half of the night, babies cycle between stages of light sleep, which is why they wake up so much more frequently, then require parental intervention” to go back to sleep.
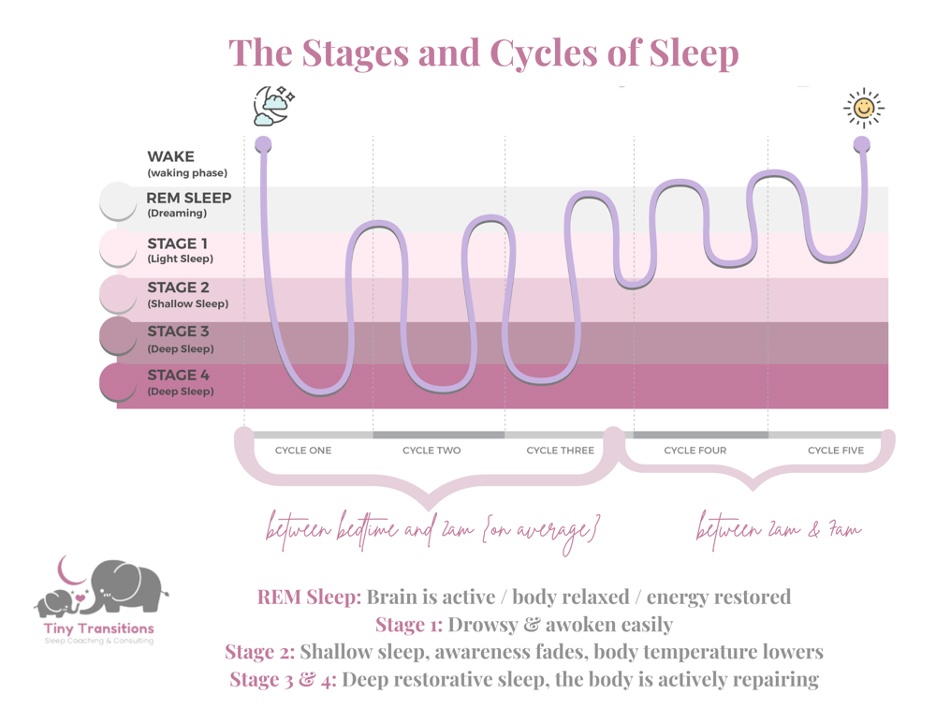
Diagram provided by Tiny Transitions
Bedtime Routines
Our experts all agree: Babies and kids thrive on routine. It can reduce anxiety because they know what’s coming next, and come to expect it. In the context of sleep (and naps), routines are so important because they signal that sleep is coming, and the body will actually start to prepare for sleep, which leads to smoother transitions.
For newborns, Desper says that “very young babies are not super aware and can’t stay awake through a lengthy routine … so this may be as simple as singing the same song before bed each night.” After a few weeks, you can start to introduce more elements like reading a familiar book, feeding, bathing and so on.
Zentz recommends a sample routine:
- Bath
- Massage with lotion
- Final feeding before bed (in just a diaper, to keep them awake and alert)
- Pajamas
- Book or song
- Rocking
- Swaddle (she especially likes the Conshy-based brand Swaddlou)
- Lay down in crib, awake
Desper recommends that, whatever elements you choose, to do them in the same order from bedtime to bedtime and from nap to nap, in order to maximize predictability. In that same vein, she even advises to head in a single “direction” until the routine is complete: “Once you go upstairs, don’t come back down and once you head into their room, don’t come back out. Heading all over the house and from room to room with your baby can be overstimulating.” The last 10 minutes of the routine should ideally be in the room the baby will be sleeping.

Naps
The newest of newborns typically won’t follow a formal sleep schedule, but understanding their cues and patterns will help build one. Remember: Wake windows rule. As Desper advises, “Stretching a baby to remain awake longer than is comfortable is a common (and logical) tactic but rarely results in more ideal naps.”
As you align to their wake windows and they get a little older, babies’ naps will consolidate — generally into three to four naps per day: “The organization of daytime sleep typically begins around 12 to 16 weeks and is complete by four to six months of age, depending on the baby,” Desper says. “That organization or consolidation process should result in at least three naps each day, with the first two being long (about 90 minutes each) and the third and/or fourth being a catnap, which serves to break up the period of wake time leading to bedtime.”
Lopez suggests this number of naps per age:
- Birth to 6 weeks: 4 to 6 naps
- 6 weeks to 10 weeks: 4 to 3 naps
- 11 weeks to 5 months: 3 naps
- 5 months to 7 months: 3 to 2 naps
- 7 months to 12 months: 2 naps
- 12 months to 3 years old: 1 nap
This varies with each child, of course. Most children transition to one nap at 14 months old, but some continue to need two naps up to 18 months old, Lopez says. By age two-and-a-half to three, most kids don’t nap anymore (though some will nap until kindergarten!).
The length of naps also changes with age. Lopez’s recommended nap lengths per age are:
- Birth to 6 weeks: 30 minutes to 4 hours
- 6 weeks to 15 weeks: 30 minutes to 2 hours
- 4 months to 18 months: 1 to 2 hours
- 18 months and up: 1 to 3 hours
Newborns don’t yet have a circadian rhythm, so part of your job is to help them establish the difference between day and night. “The best way to structure the day is to work on 12 hours of the day and 12 hours of night pattern, which is most closely aligned to their natural sleep rhythms,” Zentz says. “Working on your daily routine should always start with ensuring that the baby knows it’s daytime. Open the curtains, sing a song, flip on the lights — you want to make it a definitive ‘let’s start the day,’ versus them thinking it is still the middle of the night.”
Balancing Feeding and Sleeping
You may have heard advice that a big feed right before bed helps baby sleep longer, but the experts say that is not the case, and could actually be detrimental because using food as a sleep mechanism creates a bad habit that’ll eventually need to be eliminated, according to Zentz. Plus, “all of the advice surrounding bigger feeds, more frequent feeds, or starting solids will only improve sleep if hunger is the reason sleep isn’t going well,” Desper adds. “If, on the other hand, sleep isn’t going well because the timing, routine or environment … no amount of feeding will impact that.”
To maintain a balance between feeding and sleeping, Lopez advises to feed your child upon waking up. “In doing so, you will be feeding your little one when they are alert and well-rested, allowing them to get fulfilling feeds. This will also give them the chance to learn to fall asleep without having to be fed, and to start practicing independent sleep skills that will ultimately be essential for a good night’s sleep, and for long naps.”
Instead of timing feedings by the hour, Desper recommends focusing on the amount your baby must eat in a 24-hour period (for babies’ first year, that’s 24 to 32 ounces of breast milk or formula), and work that around their wake windows. “Feeding your baby five times a day with feeds spread two to four hours apart amounts to the same total as feeding them five times spread strictly three hours apart,” she says. “The difference is that being flexible with the space between allows for more optimal and flexible sleep timing and durations. This may not be ideal in terms of your desire for a schedule but is likely more ideal for your baby.”

Photograph courtesy of Getty Images
Sleep Regression
Once you’ve finally gotten a handle on your baby’s sleep, all of a sudden they reach a milestone and — BAM! — the dreaded sleep regression disrupts everything. (Cue collective groan from parents everywhere.)
Sleep regression is when a little one’s sleep pattern shifts from its established regimen. Though they’re typically temporary, regressions are challenging for both child and parent, and can vary in length and when they take place. They’ve been said to occur around four months, six months, eight months, 12 months, 18 months, and two years. These ages are traditionally associated with development and “milestone” moments — developing a circadian cycle, rolling over, crawling, walking, teething, etc. — which can impact sleep.
“When your brain is hard at work, it tends to disrupt sleep temporarily, until your baby masters the new skill they’ve been working on,” Lopez explains. “I look at sleep regressions as progressions, because all they mean is your baby is growing and learning new things!”
The important thing during regressions is to not panic (they, too, shall pass) and to avoid switching up routines. For example, Zentz describes: “If a baby stands, that might cause a regression for a night or two while they learn to sit back down. However, if you start to go in and lay them down, they begin to expect that … the expectation changed. Initially, they ‘needed’ you, they were stuck, our job as parents is to help. Now, they ‘want’ you, which is a habit that won’t go away … you are now laying them down every time they stand.”
Better Sleep for Parents
We’ve spent a lot of time focusing on the baby’s sleeping habits, but parents need good sleep, too. Our experts agree that keys to better sleep for parents include a consistent bedtime and wake time, a healthy diet, pre-bedtime meditation, getting sunlight exposure upon waking in the morning, and avoiding screen time in the bedroom and during those nighttime interactions with your baby.
Zentz also recommends getting your hormones checked: “A misalignment in hormone levels or overworked adrenals could cause sporadic wakings that can be fixed with nutrient supplementation,” she notes.
But let’s be honest: Getting enough sleep as a new parent is no easy feat, and could require calling in for reinforcements. “Hiring a professional postpartum doula is an option for some families and, if not, recruiting friends, family members or an occasional sitter to care for your baby so you can rest can be key,” Desper says. “Even a four-hour uninterrupted block of sleep each night will work miracles for your mood and level of functioning.”
If outside help is not an option, parents should try taking shifts. Desper offers this example: “Parent #1 might feed baby and hand them off to Parent #2, then go to bed early with black-out shades and earplugs to get that block of hours; when Parent #2 goes to bed, Parent #1 is back on duty. You can also reverse this so one parent whisks the baby away in the morning so the other can sleep in a bit later.” If that’s not an option, she says, try to have the non-feeding partner bring the baby to the feeding partner for overnight feeds, and then handle the after-feed soothing.
“Finding a way to divide the workload and maximize sleep stretches is the goal,” Desper continues. If you’re nursing, having your newborn in a bedside bassinet for overnight feedings — and side-lying — can make feedings (and transitions back to sleep) smoother. If bottle-feeding, have a cooler beside the bed with a bottle already prepared to save you a trip to the kitchen (and lets you respond to a crying, hungry baby faster).

Bed Sharing
While we’re on the topic of bed-feeding and bedside bassinets, what about the hot topic of bed sharing? All our experts (and the American Association of Pediatrics) discourage the practice. “I would not be doing my job if I told you that bed sharing with your baby is safe, because there is no safe way to do it; it increases the risk of SIDS and suffocation,” Lopez says. Zentz concurs: “The safest place for a baby is in their own space, free from padding, blankets and bumpers.”
While she agrees that bed sharing is not ideal (and does not recommend it), Desper also acknowledges that this is a reality for some families, “out of desperation or as an intentional choice,” and so part of the discussion should be how they can do it as safely as possible. “The bottom line is that parents are doing it, both proactively and reactively so let’s make that the conversation and support parents to wean from it if it is a reactive scenario or if the time has come. And let’s avoid ‘all or nothing’ conversations that lead parents to share sleep on the couch or in a recliner which is exponentially more dangerous than an intentional and prepared bed surface.”
When to Ask for Help
Ok, so this is a lot of information to digest. Even with all these recommendations, getting a good night’s sleep isn’t going to be easy. But sleep — for babies and parents — is so important to well-being, and it’s worth prioritizing it even if you’re feeling overwhelmed in new-parent survival mode.
Desper offers these “red flags” to look out for, as they may be signs that you should seek support from a professional:
- Feelings of resentment toward your baby or partner (or your parenting journey)
- Experiencing (or being at risk for) postpartum mood or anxiety issues
- Baby is struggling to eat well or gain weight due to fragmented sleep
- One or both parents can’t sleep due to anticipating wakings, worrying about sleep safety, or just because the baby is keeping them up
Put simply, if your current scenario feels unsustainable and is taking a toll on your family — that includes you, new parent! — you should consider talking to a sleep specialist. Not only are they experts who have seen it all (and use evidence-based methods), they meet families where they are and come up with an individualized, holistic solution that works for you. You don’t have to do this alone.
The Experts
Erica Desper is the founder of Confident Parenting, which based on the Main Line and now in its 10th year. Desper was inspired by her own struggle with chronic and severe sleep deprivation and the journey to recover from it. “I wished someone had been there to help me understand why sleep wasn’t working for us, what our options were to improve it and to support me through making the necessary changes. Then I realized I could give others what I hadn’t had and heal myself along the way.”
Maria Lopez is a pediatric sleep specialist, mom of three, and founder of Not a Peep, which she started in 2017. With her sleep plans, Lopez has guided hundreds of parents through the process of teaching their children to be independent sleepers. “My inspiration was none other than my non-sleeping infant, Alina, who is now 10 years old,” she tells us. “Like all the parents I work with, sleep deprivation took a toll on my mental health, on my family dynamics, and on the way I was experiencing motherhood. The decision to sleep train her has been one of my best parenting moments. Simply put, it changed my life, and I also believe that it SAVED me. Seeing how beneficial this was to our family, I immediately wanted to help others regain their life balance, by guiding them through the journey of sleep training, and by educating them about sleep.”
Courtney Zentz is a certified pediatric sleep professional, as well as a postpartum doula and certified lactation consultant. She founded Tiny Transitions in 2015, and wrote a very useful (and free) guide to newborns. Of her inspiration, she tells us: “When you leave the hospital, they make sure the baby is strapped in, and that’s about it. There was no support, village to lean on, or guidance to follow. You are raising a human and are completely unprepared. I never wanted a mother to feel like I did, lost and alone. After discovering the world of sleep consulting, I was hooked on a new mission, to serve and bring joy to families during what is supposed to be such a special time in their life.”




