
A Woman’s Guide to Heart Disease
Women are just as likely as men to get cardiovascular disease. Here’s what they can do to stay healthy.
Can heart attack symptoms differ between men and women?
Absolutely. Women don’t always present with the same symptoms—crushing chest pain and a pain that radiates down the left arm. Instead, they may experience unusual fatigue, shortness of breath, lightheadedness, nausea and upper back, shoulder or jaw pain. Unfortunately, some women ignore these symptoms. We spoke with Paulina Kiliddar, MD, a cardiologist and assistant professor of Medicine, Cardiology Division, at Drexel University College of Medicine, to better understand women’s risk factors and what they can do to prevent heart disease.
How do men and women differ when it comes to heart disease?
Men tend to develop blockages of the heart’s main arteries. Women more commonly have microvascular disease, which affects the heart’s smaller arteries. Standard tests aren’t good at detecting these smaller blockages, so women can be told they don’t have a problem even though they are experiencing symptoms of heart disease.
What other factors put women at risk for heart disease?
Not many women know they are at higher risk of heart disease later in life if they had preeclampsia or gestational diabetes while pregnant in their younger years. It’s important for women to know about this so they can take proactive steps to mitigate their risk later. Also, women are at a higher risk of heart disease once they hit menopause or if they have had radiation or chemotherapy for breast cancer. In all of these cases, it’s important they be monitored more closely for heart problems and stay vigilant about their risk factors.
Are women starting to get that they have the same risk of heart disease as men?
They are, but I think there is still a huge gap. This is especially true among minority women and those who face socioeconomic challenges. Often, heart disease is the last thing they’re worried about in their life. It’s a challenge for them to make time to focus on themselves, but I enjoy working with these women to find solutions for a healthier life.
What steps can women take to reduce their risk of heart disease?
I’m a big proponent of lifestyle modification—don’t smoke, eat a healthy diet and exercise regularly. This approach is a lot more powerful than medication. A healthier lifestyle has so many other benefits, including weight loss, better sleep and more energy to name just a few.
Do women need to advocate a little harder when it comes to their heart health?
I think they do. Too often, women’s heart problems get labeled as anxiety, stress or depression. Because of this, they end up having greater problems later. If a woman feels something isn’t right, she should speak up and take steps to get it addressed.
When to Have Your Heart Checked

Do I have a heart problem? It’s a question most people ask at some point in their lives. According to Drexel cardiologist Paulina Kiliddar, MD, “People who may want to be assessed are those with a strong family history of heart disease or those with other problems like diabetes, hypertension or high cholesterol that put them a greater risk of a heart problem.”
Determining whether someone has a heart problem begins during a heart disease risk assessment. “The first thing I talk to new patients about is their own medical history and their family’s history,” Dr. Kiliddar says. “I also discuss their risk factors, smoking history, and their eating and exercise habits. We may then check blood pressure, cholesterol, glucose levels and vitamin D among other things.”
More involved tests like a stress test or echocardiogram are often not ordered unless a red flag is raised, such as the presence of symptoms, a strong family history of heart disease, or elevated blood-test results.
Am I Having a Heart Attack?
Thanks to TV and movies, we all know how a heart attack looks, right? The man gasps, clutches his chest and falls to his knees in horrible pain. Problem is, women are just as likely to have a heart attack as men, but their symptoms may be far different:
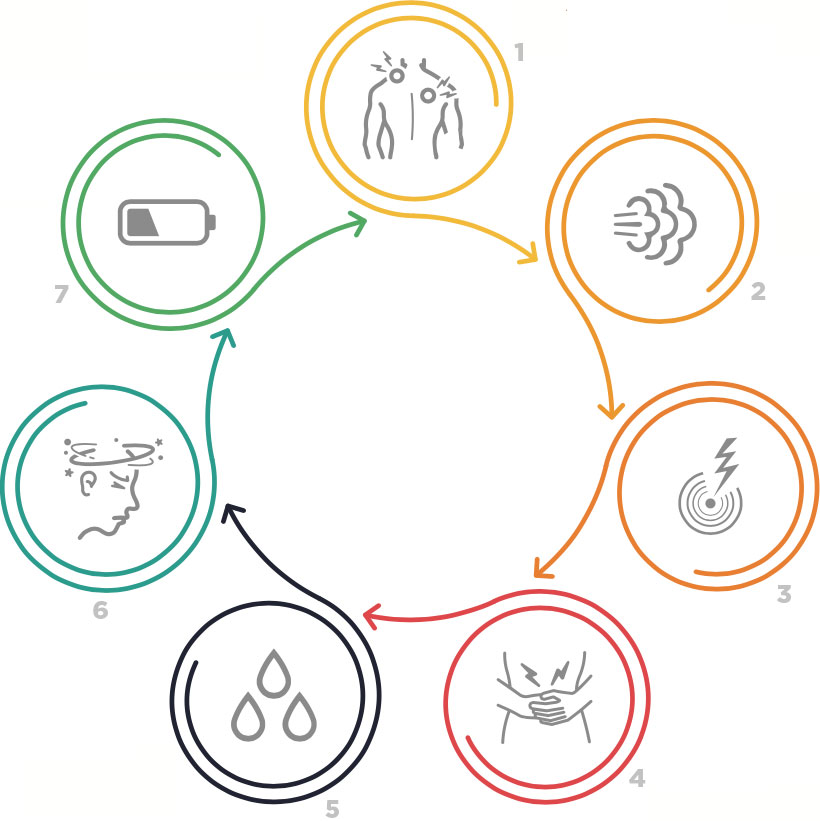
- Muscle or joint discomfort that may feel like indigestion, heartburn, fullness or squeezing.
- Shortness of breath that comes on suddenly and makes you feel like you’ve run up a flight of stairs.
- Pain in one or both arms that can’t be explained by another injury or activity.
- Nausea or vomiting that has nothing to do with what you ate or whether you’re sick
- Unusually heavy sweating that doesn’t resemble the hot flashes associated with menopause
- Lightheadedness or dizziness that may be accompanied by other non-typical symptoms
- Unusual fatigue that is unrelated to exercise and has you feeling totally wiped out
Know How to Spot a Stroke FAST
It could save a life-possibly yours.

Face drooping Does one side of the face droop or is it numb?
Arm Weakness Is one arm weak or numb? Ask the person to raise both arms. Does one arm drift downward?
Speech Difficulty Is speech slurred, is he or she unable to speak or hard to understand? Ask the person to repeat a simple sentence. Is the sentence repeated correctly?
Time to call 9-1-1 If the person shows any of these symptoms, even if the symptoms go away, call 9-1-1 and get him or her to the hospital immediately.