Here’s How the City Is Preparing to Distribute a COVID-19 Vaccine Once One Is Ready
Several vaccines for the novel coronavirus could be ready by mid-December. Here’s what — and how long — it’ll take to make them accessible to those who need them most.
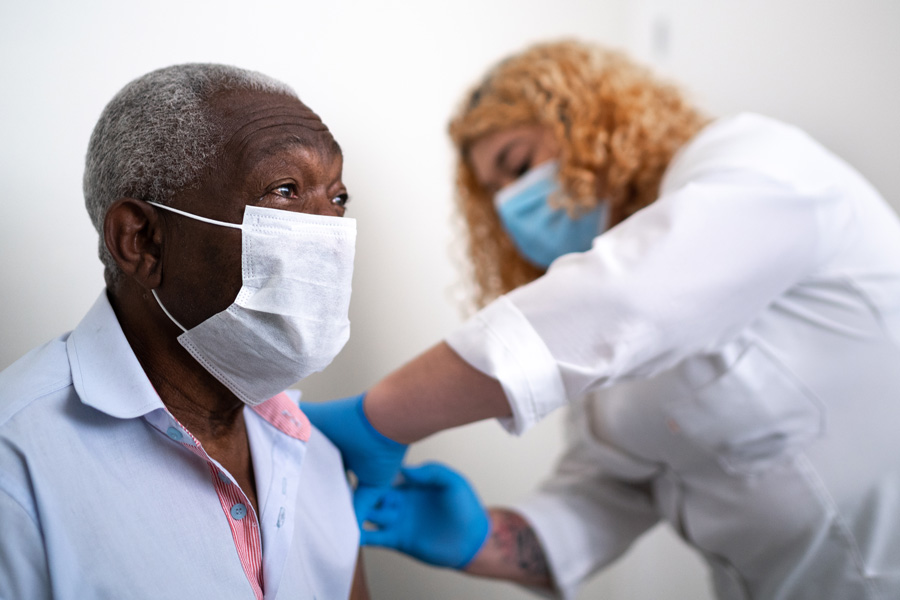
Several vaccines for the novel coronavirus could be ready by mid-December. Here’s what the vaccine distribution plans look like for Philly. Photograph by FG Trade/Getty Images
After months of clinical trials, several vaccines for COVID-19 could be ready for distribution as early as December. Moderna, the Pfizer and BioNTech team, and AstraZeneca have all announced plans to seek emergency use authorizations (EUAs) from the Food and Drug Administration after trial results showed their vaccines are safe and range from 70 percent to more than 90 percent effective against COVID-19. The FDA announced that its vaccine advisory committee will meet on December 10th to discuss the Pfizer and BioNTech EUA application and determine whether it should be approved.
“The FDA has been preparing for the review of EUAs for COVID-19 vaccines for several months and stands ready to do so as soon as an EUA request is submitted,” FDA commissioner Stephen Hahn said in a statement. “While we cannot predict how long the FDA’s review will take, the FDA will review the request as expeditiously as possible, while still doing so in a thorough and science-based manner, so that we can help make available a vaccine that the American people deserve as soon as possible.”
In response to the news, health officials have begun ramping up efforts to prepare to distribute the vaccine to populations throughout the city. It’s likely that the first available doses of the vaccine will be reserved for health-care workers and those who come in close contact with COVID-19-positive patients, but much of the city’s vaccine distribution plan is still in the works. Here’s what we’ve learned about preparations the city has made — as well as concerns some officials have about their ability to make the vaccine accessible to those who need it most.
Philly began preparing for a COVID-19 vaccine long before one was ready.
In mid-October, the Philadelphia Department of Public Health issued a draft COVID-19 Vaccine Distribution Plan documenting its tentative strategies for dispersing a COVID-19 vaccine. The plan explores everything from recruitment and training (to ensure that providers know how to properly administer the vaccine) to prioritization strategies that ensure the populations with the highest risk are protected first.
But those plans can only go so far. James Garrow, a spokesperson for the Philadelphia Department of Public Health, says the city’s plans largely hinge on guidance it has yet to receive from federal health officials about who should be prioritized to receive the vaccine, when vaccine doses will arrive in the city, what kind of vaccine the city should expect to receive, and how many doses the city should anticipate.
“The most important thing to understand about COVID-19 vaccine planning right now is that we’ve got plans, but we have outstanding questions about the most important parts of what needs to go into the plans,” Garrow explains. “All of that is dependent on the vaccine creators successfully receiving an Emergency Use Authorization from the FDA, which only one has even applied for.”
The city’s efforts will be guided by a newly established Vaccine Advisory Committee.
Last week, the city announced the establishment of its own Vaccine Advisory Committee, made up of 40 experts representing local nonprofits, academic medical centers, and city agencies who will advise the health department on planning the distribution of a COVID-19 vaccine. The idea is to get input from as many experienced, relevant voices as possible to make sure no group gets overlooked in the vaccine rollout.
As Garrow explains it, the process for any vaccine distribution begins with the Centers for Disease Control laying out guidance for how the vaccine should be distributed and who should get it first. From there, federal agencies are expected to distribute to their employees, and large health-care systems will likely receive direct shipments to distribute to staff. “It’s impossible to say if we have the infrastructure to support vaccine distribution. We have some, our partners have some, different vaccines will have different requirements, different vaccines will be available at different times, and different vaccines will go to different places and be used for different groups,” Garrow says.
Health-care workers will likely get the vaccine first.
According to Garrow, once the FDA has reviewed vaccine developers’ EUA applications, the CDC’s Advisory Committee on Immunization Practices will develop and release guidance about which populations should be prioritized to receive a vaccine. The health department believes high-risk health-care workers, like those who care for COVID-positive patients, will be among the first groups recommended. But even this group, Garrow says, will need to be broken down into smaller segments.
“Because of the large number of health-care institutions in Philadelphia, there are tens of thousands of people who could be eligible if the CDC makes a priority recommendation for health-care workers,” Garrow explains. “That’s likely too broad a group. Even nurses and doctors is too broad. We are working with health-care providers throughout Philadelphia to get a sense of the number of employees they have and also what their roles are.”
To break health-care workers into smaller segments by priority based on risk and need, the health department will work with hospitals to determine whether back-office hospital employees or only medical staff in COVID-specific wings should receive the vaccine initially. “Our targeted priority groups could come down to hospitals telling us who does what duties and what type of exposure to people who may have COVID they could have. The Vaccine Advisory Committee is thinking about whether, if we get enough [doses], we can vaccinate everyone who comes in contact with COVID patients in hospitals, and if we get less, what groups within that group would be at highest risk and need the vaccine first,” Garrow adds.
There likely won’t be enough doses of vaccine in the first batch for everybody who needs it.
It’s probable that the first disbursement of vaccine Philly receives won’t be enough to vaccinate even the priority groups of health-care workers. In addition, Garrow estimates it will be several months before enough vaccine is approved, produced and distributed to Philadelphia to ensure that the highest-priority groups are fully vaccinated and that distribution to the general public can occur. “We hope that by late spring/early summer 2021, that could be possible, but there are plenty of details that need to be worked out before we get to that point,” he says.
Vaccination could become mandatory for health-care workers.
Tony Reed, chief medical officer for the Temple University Health System, says there’s a reason institutions like his haven’t yet made COVID-19 vaccines mandatory. For one, you can’t mandate vaccination until you have enough supply. Second, Reed says, because the vaccine is so new, compulsion may not be the best approach. “I think it’s better to work through the conversation and have discussions to help people get over their fears and really try to partner with our employees and others in making this happen,” Reed explains. “And if we can get to necessary levels of herd immunity without forcing it, I would much prefer to do that.”
But Reed didn’t rule out a mandatory COVID-19 vaccine requirement for health system employees at some point in the future. “If this becomes a recurring, seasonal virus like the flu, then yes, I would see it becoming mandatory,” he says.
Reed says 60 to 65 percent of Temple employees typically volunteer to get the annual flu vaccine. From there, Reed works with managers to remind employees who haven’t gotten their flu shots to do so as soon as possible. Those reminders typically result in another 20 to 25 percent of employees getting vaccinated. For the remaining 10 to 15 percent of employees, Reed’s team facilitates conversations to remind them of the policy that requires them to wear a mask throughout flu season if they decline the flu vaccine. He anticipates that Temple will follow a similar process for the COVID-19 vaccine.
“In those conversations, we typically get to about a 92 to 95 percent rate of people accepting the vaccine and about a six percent declination rate of those who prefer to wear a mask for the winter,” Reed explains. “If COVID vaccine becomes a recurring vaccine that’s necessary repeatedly, I think it could become mandatory. Certainly, if we get the vaccine and we’re only getting 20, 30 or 40 percent vaccinated, that would mean we have a lot more messaging to do to really get people’s comfort level where it needs to be.”
Tracking the vaccine will be a huge undertaking.
Part of the health department’s role will be to ensure that the vaccine that comes to Philadelphia is properly tracked and utilized. Garrow says the tracking requirements for the COVID-19 vaccine are much stricter than for any vaccine the department has worked with since the H1N1 influenza vaccine. While the city has a great record of tracking all childhood vaccines administered in Philadelphia in its immunization registry, the COVID-19 vaccine tracking requirements could be a challenge.
“The health department has been told that we need 100 percent vaccine reporting and tracking, meaning that we need to be able to report to the CDC every single dose that is administered in Philadelphia as soon as it’s administered,” Garrow explains. “This is important because we won’t be able to order more vaccines from the CDC until we’re able to show that vaccine is being administered properly in Philadelphia. It’s also important that Philadelphia is accurately tracking COVID-19 vaccine because several of the vaccines currently in development will require two doses that could, based on the particular vaccine, need to be given at different intervals. That means some people will need to get a second dose of a particular vaccine after 21 days, and other people will need to get a second dose of a different vaccine after 28 days, and others still will only need to get one dose of a third vaccine. If we don’t track who got what and when, someone could end up getting two different vaccines or not getting a second dose that they should have.”
Garrow says the city will also be relying on vaccine tracking at the national level to guide efforts here: “The health department needs to be able to look up if someone got a particular vaccine, and when, in another county or even another state, and our data has to be available for other cities, counties and states to reference.”
Trust and willingness among the most at-risk groups will be the biggest challenge of all.
There’s no question that the most vulnerable populations in Philly should be first to receive the vaccine. Among them are African Americans, who account for more COVID-19 cases than any other race, and aging residents, particularly those 75 or older, who account for more COVID-19 deaths than any other population. These groups, says Charles Cairns, dean of the College of Medicine at Drexel University and a member of the city’s Vaccine Advisory Committee, must be prioritized to receive the vaccine first.
“I think the biggest challenge is making sure we have a plan to address those communities that have been hardest hit, and that plan has got to incorporate not just giving access to the vaccine, but also making sure we gain the trust of those communities,” says Cairns. “We have to engage with members of those communities so that we get a maximum number of people willing to take the vaccine. And then we need to be able to track people to make sure they get their follow-up shot if there’s a dosing regimen, and we need to continue to track them to make sure they’re doing well and that there are sound outcomes from the vaccination program. If we have any breakdowns in any of those areas, then I think we won’t get the vaccine in the hands of the people who need it the most.”
Najja Orr, president of the Philadelphia Corporation for Aging and a VAC member, says he’s confident the aging community will get on board when a vaccine is ready. “I think clear and frequent communication with our older-adult population is key,” he explains. “It’s important that older residents receive information about the implementation plan early on as well as regular updates as the city nears implementation. I believe a clear outreach and education plan will help to stave off any hesitancy in the aging community when that time comes.”
Ala Stanford, also a member of the VAC and founder of the Black Doctors COVID-19 Consortium, is concerned that Black people might not be prioritized in initial vaccine distribution. “I think there was this thought that if Black people don’t trust the health-care system, they shouldn’t be on a prioritized list,” Stanford says. “But not all Black people feel this way. There were many initial misconceptions, but that’s why you have a committee.”
According to Stanford, in the early days of the pandemic, tests were only being offered to health-care workers and those in the aging community. These criteria excluded many essential workers in the Black community from getting tested. Stanford worries this same type of exclusion could occur with the vaccine if other segments of the Black community aren’t prioritized. To address this issue, she has proposed vaccine prioritization by zip code, an approach she believes will ensure that people that who don’t fall into a prioritization category by profession or age aren’t overlooked. “If the positivity rates are higher in your zip code, you belong on that list to be one of the first to receive the vaccine,” she says.
Stanford is also concerned about another group within the Black community: working-class residents. “In the African American community, it’s working-class people in the 45-to-55 age range that are going out to work and bringing COVID home to their families. They need the vaccine most,” she says. “Giving the vaccine to Black people first isn’t a race-based approach; it’s evidence-based. They should be the first to get it because they’re the most affected group, which also makes them the most likely to transmit it to others. If folks don’t get the vaccine, it should be because they decided they didn’t want it, not because it wasn’t offered.”
Temple’s Reed believes trust will be a critical component in any successful vaccine distribution plan, regardless of the group to which the city is reaching out. “Our biggest concern is in vaccine willingness,” he says. “We want to be able to deliver a message in a credible way that encourages people to receive the vaccine. So we need to make sure we’re working with all of our patients, employees, neighborhoods, community leaders, and all of the groups with whom we work to really get the message out that the vaccines have gone through the FDA process the way they normally would — they just went through in a more rapid way — and that the vaccines have been demonstrated to be safe and effective and are our best chance in the fight against COVID.”


